Cancer genomics
Get a better understanding of how cancer develops and how whole genome sequencing can deliver better patient care.
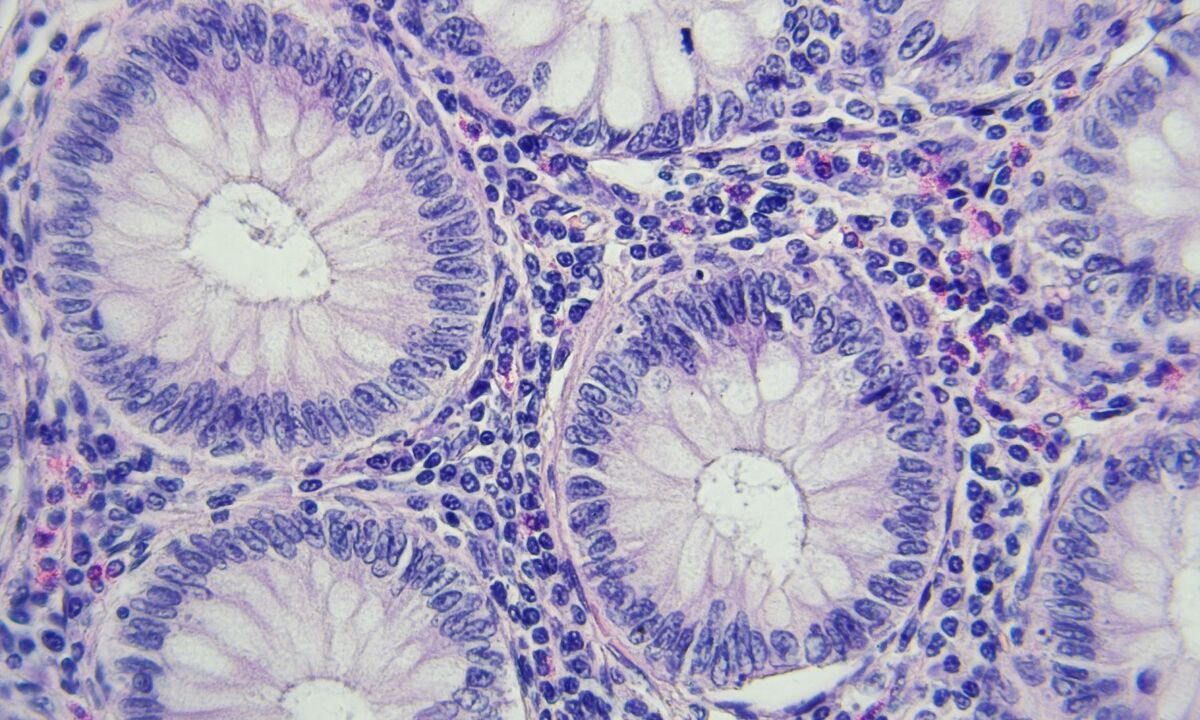
How cancer develops
Cancer starts in our cells.
Inside almost every cell of your body is a copy of your genome, made of DNA. The genome can be thought of as the instructions for running a cell. It tells the cell what kind of cell to be – is it a skin cell or a liver cell? It also has the instructions that tell the cell when to grow and divide, and when to die.
When a cell divides to become two cells, your genome is copied. Usually, our cells divide to make new cells in a controlled way. This is how our bodies grow and repair.
Sometimes when our cells divide, mistakes happen when copying the genome. These are called mutations. They are caused by natural processes in our cells, or just by chance. They can be caused by external factors in our environment too – like radiation from sunlight.
Usually, cells can repair mutations in their genome. In fact most DNA damage is repaired immediately, with no ill effects. If the damage is very bad, cells may self destruct instead. Or the immune system may recognise them as abnormal and kill them. This helps to protect us from cancer.
But sometimes mutations in critical genes mean that a cell no longer understands its instructions, and starts to multiply out of control. It doesn’t repair itself properly, and it doesn’t die when it should. The abnormal cell keeps dividing and making more and more abnormal cells. These cells form a lump, which is called a tumour.
When we sequence DNA from cancer patients, we use DNA from both the tumour and healthy cells so we can compare the two.
Whole genome sequencing for cancer
Cancer whole genome sequencing allows us to detect two types of changes, germline mutations and somatic mutations.
Germline mutations
These are changes that are inherited from one's parents, or that occur spontaneously in very early development of the foetus.
These changes to the genome don’t match the human reference genome that we use for a guide.
They are often passed down through generations. They can affect a person's chances of developing cancer, for example changes in the BRCA1 and BRCA2 genes can lead to an increased risk of breast and ovarian cancers. We look for these changes if they are thought to be the cause of someone’s cancer.
We can also look for these changes in patients who don’t have cancer – but only if they want us to. In this case these are called ‘additional findings’.
Somatic mutations
These are changes that occur in the genome of cancer cells. Somatic mutations can be caused by environmental factors. For example, damaging UV rays from the sun cause changes of the C base in DNA to a T, which can lead to tumour formation. These can be detected by whole genome sequencing, by comparing the sequence from a patient’s sample and the sequence from a sample of their tumour.
We can also detect changes to the cancer genome caused by a range of other environmental factors, such as smoking, and viral infections, or the random changes that occur when a cancer is rapidly expanding.
Patient care
We sequence the DNA from a patient’s tumour and healthy cells and compare the two sequences. This gives insight into the exact nature and genomic changes that are causing an individual’s cancer and can:
Improve diagnosis
using increasingly advanced DNA-deciphering genomics technologies
Help clinicians select the most effective treatments
based on the genomic data of the patient
Show which patients are likely to benefit from clinical trials
based on their genomic data
Familial breast cancer
An example of the benefits of cancer genomics
Familial breast cancer is caused by abnormal genes passed from parent to child. Families that have familial breast cancer may have men with breast cancer and sometimes have other cancers, such as ovarian cancer or prostate cancer. In these families, cancers may develop at a younger age than usual.
1 in 8
women in the UK affected by breast cancer
5-10%
of breast cancers are thought to be hereditary
Familial breast cancer and the BRCA genes
Most inherited cases of breast cancer are associated with specific changes in two genes: BRCA1 (BReast CAncer gene one) and BRCA2 (BReast CAncer gene two).
Everyone has BRCA1 and BRCA2 genes. The function of the BRCA genes is to repair cell damage and keep breast cells growing normally. But when these genes contain abnormalities or mutations, the genes don’t function normally and breast cancer risk increases.
Doctors are increasingly likely to use information about a patient’s BRCA status, together with lots of other information, to help determine which drug to prescribe. We hope that, one day, treatments based on the specific characteristics of the tumour, including the genetic make-up, can be offered to all patients.

The benefit of genomics in breast cancer
It's important to note that not all familial breast cancer is due to mutations in BRCA. Changes in other genes have also been found which have a role in causing familial breast cancer. And research might identify still more. There is also a lot of research into how to use genomic testing to predict long term prognosis for breast cancer patients, and how it could be used to guide treatment and screening.
Finding an inherited mutation responsible for a cancer means that other family members could then be tested for it, if they wished to be. This would help predict their risk, and preventative surgery may be an option for some people.
The ability to prevent and identify gene mutations in order to save and change the lives of patients is what genomic medicine is all about.

Support for those affected by cancer
Each of these charities or support organisations can provide information, support or services for families affected by cancer.
Breast Cancer Now provides support and access to research insights and healthcare professionals
-
Cancer Research UK has information and resources on types of cancer and research happening across the UK
-
Macmillan Cancer Support offers support and an online community for those diagnosed with cancer and their families
-
Target Ovarian Cancer gives you access to an online community of others affected by ovarian cancer, as well as information and support events
-
Cancer Support UK provides practical and emotional support to people with cancer, during and after the treatment period
-
Maggie's has free cancer support and information in centres across the UK and online
-
Children with Cancer UK lends support to families and children with cancer
Participant stories
Find out how genomic medicine has impacted the lives of participants.